Researchers at the Leiden Academic Centre for Drug Research(LACDR) have continued to test their models to enhance the testing and development of cancer immunotherapies. Using 3D bioprinting technology, they create mini-tumors in a collagen gel that closely mimics human tissue. This method allows them to observe real-time interactions between these mini-tumors and immune cells, providing a more accurate assessment of the efficacy of cancer treatments.
Revolutionizing Cancer Treatment
Cancer cells often evade detection by the immune system, making it challenging for conventional therapies to target and eliminate them. Immunotherapy, which helps the immune system recognize and destroy cancer cells, is a promising approach. It involves enhancing T-cells, specialized immune cells that attack cancer cells, or using bispecific antibodies that bind to both T-cells and cancer cells, guiding the immune response more effectively. The Leiden researchers are testing strategies for these approaches, moving beyond traditional methods that rely on petri dishes, which fail to capture the complexity of the human body.
A More Realistic Model
The team’s new method involves 3D-printing mini-tumors embedded in a collagen gel. This gel mimics the structure of human tissue, allowing tumors to grow and invade the gel, much like real tumors in the body. Enhanced T-cells are then added to the model, which must navigate their way to the tumors, simulating the real-life scenario. This high-throughput method enables researchers to test various T-cells and antibodies more effectively.
Additionally, the researchers use automated microscopes to monitor these interactions in real-time. This setup allows them to observe not only the effectiveness of the enhanced T-cells and antibodies but also the defense strategies used by the tumor cells.
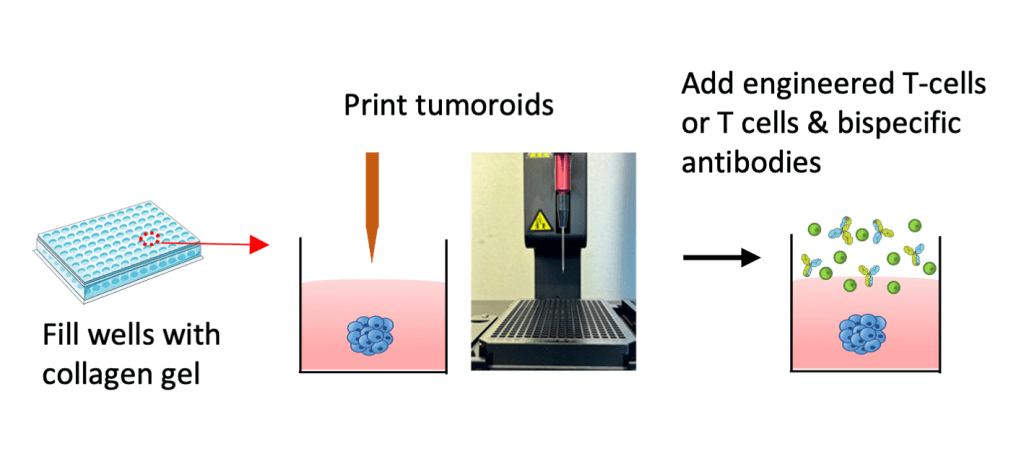
A 3D bioprinter creates small, three-dimensional tumours in a collagen gel that continue to grow. The researchers then add T-cells and observe what happens. Image: Liao et al. (2024)
Promising Results and Future Applications
This new model has already demonstrated its utility in testing bispecific antibodies, revealing that some antibodies previously thought effective did not perform well in this more complex environment. The research team is also using their model to evaluate improved T-cell receptors for specific cancers, including breast and eye cancers. Collaborating with other experts, they have successfully predicted which receptors will be effective in mouse models, paving the way for clinical trials in human patients. This breakthrough represents a significant step forward in selecting optimal treatments for cancer patients, bringing hope for more effective therapies in the future.
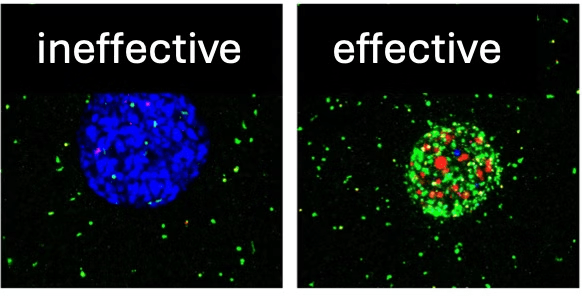
A tumor to which inactive (left) and active (right) antibodies have been added. Green indicates T-cell recruitment, red indicates tumor killing. Image credit: Liao et al. (2024).
About LACDR
The Leiden Academic Centre for Drug Research (LACDR) is a leading research institute at Leiden University in the Netherlands, dedicated to advancing drug discovery and development. It focuses on understanding the mechanisms of disease, designing novel therapies, and developing innovative drug delivery systems. With a strong emphasis on interdisciplinary research, LACDR collaborates with global academic and industry partners to translate scientific discoveries into effective treatments, particularly in areas like cancer, neurodegenerative diseases, and infectious diseases.
References:
Liao, CY., Engelberts, P., Ioan-Facsinay, A. et al. CD3-engaging bispecific antibodies trigger a paracrine regulated wave of T-cell recruitment for effective tumor killing. Commun Biol 7, 983 (2024). https://doi.org/10.1038/s42003-024-06682-9.
Kortleve, D. et al.. TCR-engineered T-cells directed against Ropporin-1 constitute a safe and effective treatment for triple-negative breast cancer. Cancer Discov 2024; https://doi.org/10.1158/2159-8290.CD-24-0168
Header image: A tumour attacked by T-cells in the assay. Blue and Red: nuclei and cytoskeleton of the tumour cells. Green: T-cells. Image: Liao et al. (2024), Nature communications biology, doi: 10.1038/s42003-024-06682-9.




Leave a comment